Diabetes Type 1: Know The Type 1 Diabetes Symptoms

Although type 1 diabetes can occur at any age, it is more common before the age of 40 and frequently occurs during childhood. Type 1 diabetes accounts for only 10% of all diabetes cases. Type 1 diabetes causes the pancreas, a tiny gland behind the stomach, to gradually stop making insulin. Insulin is the hormone that regulates blood glucose levels. Over time, too much glucose in the blood can harm the body’s organs.
Diabetes type 1 causes
The immune system, the body’s natural defense against disease and infection, misidentifies the cells in your pancreas as dangerous, resulting in type 1 diabetes.
Without insulin, your body will begin metabolizing fat and muscle, causing you to lose weight. This can lead to diabetic ketoacidosis, a potentially fatal short-term condition. The bloodstream becomes acidic at this stage, and you experience dangerously high blood ketone levels and acute dehydration.
As a result, your body cannot produce insulin, which is required to carry glucose from your blood to your cells, where it may be used as fuel. Type 1 diabetes is the most common type.
Type 1 diabetes symptoms
The type 1 diabetes symptoms listed below are common. Some people with diabetes, however, have symptoms that are so subtle that they go untreated.
Typical type 1 diabetes symptoms include:
- urine regularly
- feeling extremely hungry despite eating, tremendous exhaustion
- cloudy vision
- Bruises/cuts that are difficult to heal
- Weight loss despite eating more (type 1)
- Tingling, pain, or numbness in the hands or feet of type 2
Diabetes complications can be reduced with early detection and treatment.
Type 1 and type 2 diabetes have many symptoms, but their fundamental causes differ. Furthermore, treatment is frequently inconsistent. When symptoms of type 1 and type 2 diabetes overlap, it can be confusing, especially in adults recently diagnosed with type 1 diabetes.
Treatment for type 1 diabetes
It is critical to diagnose diabetes as soon as possible. If left untreated, type 1 diabetes poses a major threat to life. Early intervention with therapy is critical. Diabetes cannot be cured, but therapy aims to control symptoms and keep blood glucose levels as close to normal as possible to avoid health problems later in life.
If you are diagnosed with diabetes, you will be referred to a diabetes care team for expert treatment and monitoring. Because your body cannot produce insulin, you require daily insulin shots to maintain normal glucose levels. You’ll learn how to do this and alter your insulin dosage based on your blood glucose level, the amount of exercise, and the carbohydrates you consume.
Insulin injections come in various forms, each of which works slightly differently. Most likely, you’ll need a combination of insulin formulations. Some individuals are given quick-acting insulin by continuous infusion (pump therapy). In this case, a tiny device constantly injects insulin into your bloodstream at a rate you control via a plastic tube (cannula) inserted under the skin with a needle.
Complications
Diabetes, if left untreated, can cause a range of health problems. High glucose levels can injure organs, neurons, and blood vessels.
A chronically raised glucose level that produces no symptoms can cause long-term harm.
Issues may arise if your diet and exercise do not properly regulate your insulin. You will work with your diabetes care team to correctly control your insulin.
Wrapping Up
Adults with diabetes are sometimes mistaken as having type 2 diabetes. This could be because some healthcare providers are ignorant that type 1 diabetes can develop at any age and in people of different races, colors, shapes, and sizes. People with type 1 diabetes who have high blood glucose levels and traditional risk factors for type 2 diabetes, such as being overweight or inactive, are frequently misdiagnosed. It can also be problematic because some persons with newly diagnosed type 1 diabetes have no symptoms at first. During a routine appointment, their doctor discovers a high blood glucose level and recommends diet, exercise, and oral medicine.

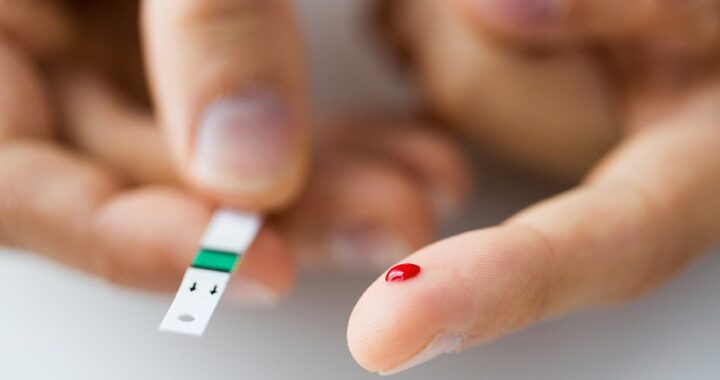 Key Features of Prediabetes App
Key Features of Prediabetes App 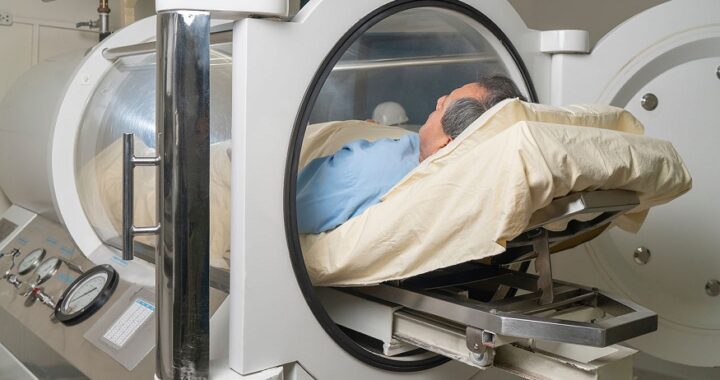 Hyperbaric Oxygen Therapy in Reproductive Medicine
Hyperbaric Oxygen Therapy in Reproductive Medicine  The Aesthetic and Functional Benefits of Compression Gear
The Aesthetic and Functional Benefits of Compression Gear  Types Of Physical Activities You Can Undertake From Today
Types Of Physical Activities You Can Undertake From Today 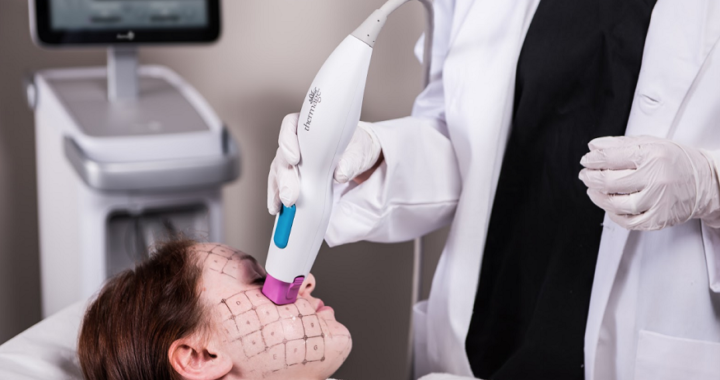 Why Is Thermage FLX So Expensive in Singapore
Why Is Thermage FLX So Expensive in Singapore